Compassion fatigue: Tools for Resiliency Program
12th September 2019

Animal Shelter Work: Rewarding and Stressful
Working within the animal shelter context can be extremely rewarding. Animal shelter personnel frequently report their work with animals as a calling and derive a strong sense of satisfaction from being able to ease suffering, rehome and rehabilitate animals under their care (Rohlf & Bennett, 2005). The work, however, can also be stressful with animal shelter personnel consistently reporting high levels of guilt, sadness, anger, exhaustion, and burnout resulting from their work (Frommer & Arluke, 1999; Hart & Mader, 1995; Scotney, 2015).
Prolonged exposure to animal suffering, neglect and abuse together with working in sometimes aversive work conditions (e.g., aversive smells, loud noise, bites and risk of zoonotic disease transmission) place animal shelter personnel at risk of occupational stress (Hart & Mader, 1995; Rohlf & Bennett, 2005; Scotney, 2015). The euthanasia of animals is particularly distressing with many reporting job strain, sadness, anger, depression, and traumatic stress symptoms including intrusive thoughts, difficulty sleeping and nightmares in response to participating in the procedure (Anderson, Brandt, Lord, & Miles, 2013; Baran et al., 2012; Reeve, Rogelberg, Spitzmuller, & DiGiacomo, 2005; Rohlf & Bennett, 2005). This form of stress affecting animal shelter personnel has been collectively referred to as compassion fatigue (Rohlf, 2018; Scotney, 2015).
 What is Compassion Fatigue?
What is Compassion Fatigue?
Compassion Fatigue (CF) was first coined by Joinson (1992) to describe a unique form of burnout affecting professional caregivers. It is thought to be the result of extended and intense interactions with patients or victims of trauma, the use of self and cumulative exposure to stress (Coetzee & Klopper, 2010). Although there are conflicting definitions of compassion fatigue in the literature, Killian (2008) and Stamm (2010) state the condition encompasses both Secondary Traumatic Stress (STS) and burnout. The former is a stress reaction caused by secondary or indirect exposure to trauma. The symptoms of STS include avoidance of reminders, emotional numbing, and intrusive thoughts or images associated with the event (Figley, 2013). Burnout is thought to be caused by continuous exposure to workplace stressors and is characterised by exhaustion, disengagement, cynicism, and feelings of sadness and overwhelm (Maslach, 2003; Stamm 2010).
Compassion fatigue negatively impacts the wellbeing of animal shelter personnel and can lead to negative implications on the individual and the organisation. The condition has been linked to an increased risk of accidents (Trimpop, Kirkcaldy, Athanasou, & Cooper, 2000), an exacerbation of mental health disorders including anxiety and depression, and an increased risk of suicide (Bartram, 2010; Bartram, Yadegarfar, & Baldwin, 2009; Tiesman et al., 2015). In an organisational context, compassion fatigue can contribute to staff turnover and decreased workplace performance. For example, in critical care nurses and surgeons, compassion fatigue is linked with self-reported medical errors (Maiden, Georges, & Connelly, 2011; Shanafelt et al., 2010) and self-reported decreased quality of patient care (Boamah, Read, & Spence Laschinger, 2017). Although no research exists investigating the link between compassion fatigue and animal welfare, these results suggest that compassion fatigue may have deleterious effects on animal welfare outcomes.
The Need for Compassion Fatigue Resiliency Programs
These negative workplace and individual implications make the availability of effective therapeutic interventions in the animal shelter environment increasingly important. A recent review of current compassion fatigue interventions for animal care professionals indicates that, although occupational stress is highly prevalent in this population, very few evaluated intervention programs exist (Rohlf, 2018). Based on this review, Rohlf (2018) recommends that programs which incorporate psychoeducation, coping skills training and relaxation within a cognitive-behaviour framework are useful starting points with which to base future compassion fatigue interventions.
Responding to the need for interventions for these dedicated animal care professionals and using the knowledge gained from an extensive literature review, the Compassion Fatigue – Tools for Resilience program was developed.
Compassion Fatigue – Tools for Resiliency Program
The program can be delivered as a 90-minute seminar, half day or full day workshop and is delivered to group sizes ranging from 8 to 15. A modified version of this program has also been successfully delivered to other animal care sectors including research facilities, zoos, and wildlife rescue.
The program content is delivered in an interactive manner. Recognising participants as experts in their own working lives this workshop utilises group discussion and feedback as part of its content. Taking the half day workshop as an example, the following areas are covered:
- Self-awareness. Self-awareness is fostered through discussion of the signs and symptoms of compassion fatigue, risk and protective factors of the condition and early warning signs.
- Distress reduction and emotion regulation. Attendees learn strategies to reduce distress and promote emotion regulation and relaxation.
- Building resilience. Group members learn skills to build resilience through reframing and solution focused therapy exercises. Attendees as also shown ways to promote compassion satisfaction and self-compassion, key protective factors of compassion fatigue (Alkema, Linton, & Davies, 2008; Dombo & Gray, 2013; Duarte & Pinto-Gouveia, 2017; Thieleman, Cacciatore, & Hill, 2014).

Does the Program Work?
As part of RSPCA Victoria’s people strategy, I’ve been working with their staff and volunteers and it has been both a privilege and a pleasure to work with these dedicated, skilled and compassionate people. The compassion fatigue resiliency program is one of the many ways RSPCA Victoria looks after their staff placing them as an employer of choice.
The feedback in response to this program is overwhelmingly positive. For example, a recent evaluation of the half day workshops revealed significant increases in compassion fatigue knowledge and perceived confidence in coping with workplace stress based on comparisons between pre and post workshop survey results.
Most participants from this evaluation rated opportunities for discussion with peers (78.0%), the usefulness of content (85.3%), the teaching style of the facilitator (95%), the workshop overall (88.5%) as very good to excellent.
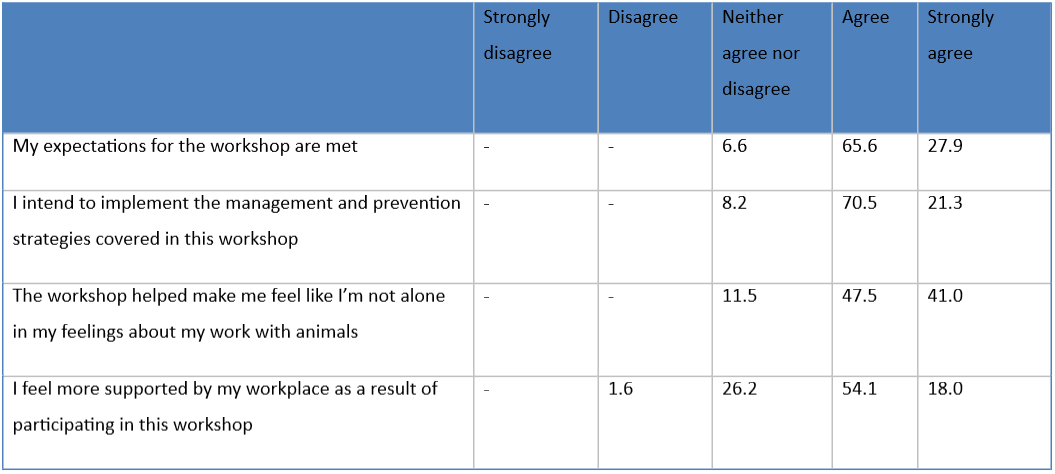
Table 1 shows that the majority of participants reported that they agree or strongly agree that their expectations for the workshop were met (93.5%), that they intend to implement the prevention and management strategies covered in the workshop (91.8%) and that participating in the workshop helped make them feel like they are not alone in their feelings about their work with animals (88.5%). Most participants also reported that they feel more supported by their workplace as a result of participating in the workshop (72.1%).
Table 1.
Percentage Ratings of Degree to which Workshop Met Expectations, Intentions to Implement Strategies, and Impact on Perceived Levels of Support.
The qualitative feedback received from this workshop was equally positive and revealed that the opportunities provided for discussion with peers and skills practice are highly valued and thought-provoking. One participant reported, “…you definitely helped me out a lot and gave me a lot to think about”. Another says “…I feel more confident in recognising compassion fatigue in myself and my peers.” Others reported a good rapport with the facilitator “Vanessa was great, very understanding and kind.”

What does this mean for your shelter?
The Compassion Fatigue – Tools for Resiliency program is an effective means of psychoeducation. This group-based intervention is also helpful in engaging staff in discussions around the topic of compassion fatigue, fosters peer support within the workplace and allows members an opportunity to normalise and reflect on how their work with animals impacts their lives. Compassion fatigue cannot, of course, be eradicated by one-off participation in a workshop. This intervention program should ideally be part of a broader resiliency and wellbeing program which builds on and reinforces skills learnt including refresher courses, coping skills training, individual counselling and group debriefing sessions. Consultation in regard to workplace procedures and policies which promote compassion fatigue resiliency is also recommended.
Special thanks to Erin Dann (Head of People and Culture – RSPCA Victoria) for her dedication to supporting the wellbeing of RSPCA Victoria employees by overseeing and coordinating the Compassion Fatigue Resiliency programs. I would also like to extend gratitude to Dr. Liz Walker (CEO – RSPCA Victoria) for her commitment to prioritising the health and wellbeing of RSPCA Victoria employees.
If you’d like to run a workshop at your workplace or have questions about compassion fatigue resiliency, please contact Dr. Vanessa Rohlf, certified compassion fatigue therapist and educator at virohlf@gmail.com
References
Alkema, K., Linton, J. M., & Davies, R. (2008). A study of the relationship between self-care, compassion satisfaction, compassion fatigue, and burnout among hospice professionals. Journal of Social Work in End-of-Life & Palliative Care, 4(2), 101-119.
Anderson, K. A., Brandt, J. C., Lord, L. K., & Miles, E. A. (2013). Euthanasia in Animal Shelters: Management’s Perspective on Staff Reactions and Support Programs. Anthrozoös, 26(4), 569-578. doi:10.2752/175303713X13795775536057
Baran, B. E., Rogelberg, S. G., Carello Lopina, E., Allen, J. A., Spitzmüller, C., & Bergman, M. (2012). Shouldering a silent burden: The toll of dirty tasks. Human Relations, 65(5), 597-626. doi:10.1177/0018726712438063
Bartram, D. J. (2010). Veterinary surgeons and suicide: a structured review of possible influences on increased risk. The Veterinary record, v. 166(no. 13), pp. 388-397-2010 v.2166 no.2013. doi:10.1136/vr.b4794
Bartram, D. J., Yadegarfar, G., & Baldwin, D. S. (2009). A cross-sectional study of mental health and well-being and their associations in the UK veterinary profession. Social psychiatry and psychiatric epidemiology, 44(12), 1075.
Boamah, S. A., Read, E. A., & Spence Laschinger, H. K. (2017). Factors influencing new graduate nurse burnout development, job satisfaction and patient care quality: a time-lagged study. Journal of advanced nursing, 73(5), 1182. doi:10.1111/jan.13215
Coetzee, S. K., & Klopper, H. C. (2010). Compassion fatigue within nursing practice: A concept analysis. Nursing & health sciences, 12(2), 235-243.
Dombo, E. A., & Gray, C. (2013). Engaging spirituality in addressing vicarious trauma in clinical social workers: A self-care model. Social Work and Christianity, 40(1), 89.
Duarte, J., & Pinto-Gouveia, J. (2017). Mindfulness, self-compassion and psychological inflexibility mediate the effects of a mindfulness-based intervention in a sample of oncology nurses. Journal of Contextual Behavioral Science, 6(2), 125-133.
Frommer, S. S., & Arluke, A. (1999). Loving Them to Death: Blame-Displacing Strategies of Animal Shelter Workers and Surrenderers. Society & Animals, 7(1), 1-16. doi:10.1163/156853099X00121
Hart, L. A., & Mader, B. (1995). Pretense and hidden feelings in the human society environment: A source of stress. Psychological Reports, 77(2), 554-554. doi:10.2466/pr0.1995.77.2.554
Joinson, C. (1992). Coping with compassion fatigue. Nursing, 22, 116–120.
Killian, K. D. (2008). Helping till it hurts? A multimethod study of compassion fatigue, burnout, and self-care in clinicians working with trauma survivors. Traumatology, 14(2), 32-44.
Maiden, J., Georges, J. M., & Connelly, C. D. (2011). Moral distress, compassion fatigue, and perceptions about medication errors in certified critical care nurses. Dimensions of Critical Care Nursing, 30(6), 339-345.
Maslach, C. (2003). Burnout: The cost of caring. Cambridge MA: Malor Books.
Reeve, C. L., Rogelberg, S. G., Spitzmuller, C., & DiGiacomo, N. (2005). The caring-killing paradox: euthanasia-related strain among animal-shelter workers.(Author Abstract). Journal of Applied Social Psychology, 35(1), 119.
Rohlf, V., & Bennett, P. (2005). Perpetration-induced Traumatic Stress in Persons Who Euthanize Nonhuman Animals in Surgeries, Animal Shelters, and Laboratories. Society & Animals, 13(3), 201-220. doi:doi:https://doi.org/10.1163/1568530054927753
Rohlf, V. I. (2018). Interventions for occupational stress and compassion fatigue in animal care professionals—A systematic review. Traumatology, 24(3), 186-192. doi:10.1037/trm0000144
Scotney, R. L. (2015). A systematic review of the effects of euthanasia and occupational stress in personnel working with animals in animal shelters, veterinary clinics, and biomedical research facilities. Journal of the American Veterinary Medical Association, v. 247(no. 10), pp. 1121-1130-2015 v.1247 no.1110. doi:10.2460/javma.247.10.1121
Shanafelt, D. T., Balch, M. C., Bechamps, J. G., Russell, J. T., Dyrbye, J. L., Satele, J. D., . . . Freischlag, J. J. (2010). Burnout and Medical Errors Among American Surgeons. Annals of surgery, 251(6), 995-1000. doi:10.1097/SLA.0b013e3181bfdab3
Stamm, B. (2010). The concise manual for the professional quality of life scale. Retrieved from https://proqol.org/uploads/ProQOL_Concise_2ndEd_12-2010.pdf
Thieleman, K., Cacciatore, J., & Hill, P. W. (2014). Traumatic bereavement and mindfulness: A preliminary study of mental health outcomes using the ATTEND model. Clinical Social Work Journal, 42(3), 260-268.
Tiesman, H. M., Konda, S., Hartley, D., Chaumont Menéndez, C., Ridenour, M., & Hendricks, S. (2015). Suicide in U.S. Workplaces, 2003-2010: a comparison with non-workplace suicides. American journal of preventive medicine, 48(6), 674-682. doi:10.1016/j.amepre.2014.12.011
Trimpop, R., Kirkcaldy, B., Athanasou, J., & Cooper, C. (2000). Individual differences in working hours, work perceptions and accident rates in veterinary surgeries. Work & Stress, 14(2), 181-188. doi:10.1080/026783700750051685




